Is it Possible to Reverse Afib Naturally?

Atrial fibrillation, also known as Afib, affects millions worldwide, causing irregular and rapid heartbeats that can lead to serious complications like stroke and heart failure. While medications and procedures are commonly used to manage Afib, many individuals try natural approaches to alleviate symptoms and potentially reverse the condition.
How Long Will My Pacemaker Last?
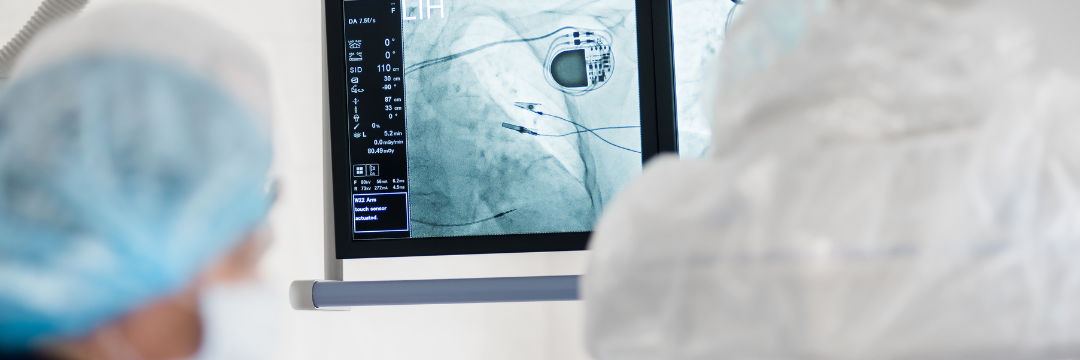
Many patients needing a pacemaker or with a recent pacemaker implant are concerned about the durability of the pacemaker’s pulse generator or battery. How long will it last? While we cannot predict exactly when the battery will finally stop, patients can expect, on average, between eight and ten years out of their pacemaker.
Sleep Apnea and Afib

Atrial fibrillation, also called Afib, affects over 33 million people worldwide. It is the most common irregular heartbeat (arrhythmia). Almost 40 million US adults have obstructive sleep apnea in the US alone. Both conditions increase the risk of stroke and death. Research has shown a connection between Afib and sleep apnea.
Sleep apnea disrupts breathing during sleep. Alternately, sleep apnea can lead to shallow breaths. Either disrupts the natural rhythm of sleep. There are two primary types of sleep apnea: obstructive sleep apnea (OSA), which is from a physical airway obstruction, and central sleep apnea (CSA), which disrupts the brain’s respiratory control.
The Role of Statins in Treating and Preventing Afib
Atrial fibrillation, also called Afib or AF, affects over 33 million people worldwide. Afib is an irregular (arrhythmia) and often rapid heartbeat that can lead to many complications, including stroke and heart failure. Recent studies have shown that statin drugs – usually prescribed for high cholesterol – may help treat and prevent Afib.
The Types of Afib and What It Means For Your Care

As you undoubtedly know by navigating our website, atrial fibrillation of Afib is a very concerning condition that affects millions of adults around the United States and is increasing in prevalence with the commensurate increase in excess weight and metabolic disease. Concerningly, because many patients do not understand the progression of the condition, some do not seek care early enough and may progress to a more severe stage of Afib. This progression is not necessarily linear. For some, it may occur within months, while others may take years. Ultimately, however, it becomes more challenging to treat as Afib progresses. In this article, we will talk about the various stages of Afib and the success of treatments once a patient has crossed each threshold.
Does Magnesium Prevent or Improve Afib?

Magnesium is one of those nutrients that can significantly affect our health, yet it remains underappreciated and less known among patients. Because of its beneficial effects on muscle, of which the heart is one, magnesium has been posited as a potential preventative measure or treatment for atrial fibrillation / Afib. However, does science support this claim, and should patients consider supplementing to improve heart health?
Can Weight Loss Drugs Like Wegovy® & Zepboundtm Help Afib?
Atrial fibrillation is a widespread and growing concern, with over 5 million Americans estimated to be suffering from the condition. From anecdotal evidence, there may be far more than this number. While Afib itself is rarely dangerous unless you have significant underlying cardiovascular disease, the consequences of untreated or undertreated Afib include a five times increased risk of stroke and a significantly increased risk of heart attack. Over the long term, there is an increased risk of congestive heart failure as the heart essentially tires out with all the excess and erratic beats.
But can a new class of weight loss drugs – Semaglutides (Wegovy®) and Liraglutides (ZepboundTM) or GLP-1 receptor agonists, be the answer or at least improve the symptoms of atrial fibrillation? The short answer is, possibly. Let’s dig a little deeper:
Stress Reduction Techniques to Minimize Afib

No matter how hard we try to keep our cool, some stress always seems to be associated with family, work, friends, or finances. Even with the best-made plans, there will be hurdles to jump. It’s a fact of life. However, the stress that comes with these concerns can induce or worsen an Atrial Fibrillation or Afib episode. So, what can be done to reduce this likelihood and keep your heart in top shape?
What Is a CHA2DS2-VASc Score?
 Stroke risk in Afib patients is evaluated in part with the CHA2DS2-VASc Score. As you have likely read elsewhere on this website, Atrial Fibrillation or Afib is a significant concern in the US population, with an estimated five million people suffering from its effects. While Afib itself can be at best annoying and at worst debilitating, the true risk of Afib is the five times increased chance of stroke if left untreated. While we have many treatment options, we must stratify that risk, as not all patients are the same, and some may require earlier intervention than others. As a result of this need, the CHADS2 score was created. It is a scoring methodology based on several factors that increase the risk of stroke. More recently, a new and updated version known as CHA2DS2-VASc has become our most accurate risk stratification tool, offering more precise results for low-risk patients than its predecessor.
Stroke risk in Afib patients is evaluated in part with the CHA2DS2-VASc Score. As you have likely read elsewhere on this website, Atrial Fibrillation or Afib is a significant concern in the US population, with an estimated five million people suffering from its effects. While Afib itself can be at best annoying and at worst debilitating, the true risk of Afib is the five times increased chance of stroke if left untreated. While we have many treatment options, we must stratify that risk, as not all patients are the same, and some may require earlier intervention than others. As a result of this need, the CHADS2 score was created. It is a scoring methodology based on several factors that increase the risk of stroke. More recently, a new and updated version known as CHA2DS2-VASc has become our most accurate risk stratification tool, offering more precise results for low-risk patients than its predecessor.
This scoring system is used to develop risk status for patients and inform a treatment plan for Afib. It includes the following risk factors.
Atrial Fibrillation (Afib) Diagnosis – Should You Be Worried?
It’s always worrisome to get a new diagnosis, especially when it has to do with your heart. A common heart condition that you may have heard of is atrial fibrillation or AFib. Afib is more prevalent than many think. About five million Americans have it, and it is newly diagnosed in over 200,000 new patients every year – many more may go undiagnosed. AFib is not life-threatening in and of itself, but if it goes unnoticed and unmanaged, it can cause other, more severe heart conditions to develop.